This evidence map helps healthcare readers interpret octenidine dihydrochloride evidence while keeping substance names, product labels, and individual studies separate from clinical protocols.
It is not a dosing guide, product recommendation, substitution guide, wound-care instruction, decolonization protocol, catheter-care procedure, or statement that octenidine should replace another antiseptic. Patient-specific decisions belong with local protocols, current product labeling, antimicrobial stewardship processes, infection prevention teams, and qualified clinical judgment.
Quick Position
The current clinical evidence is mixed and highly context-specific. The strongest broad source for octenidine dihydrochloride in healthcare-associated infection contexts is a 2023 review that searched Medline, Scopus, and Cochrane through August 21, 2022 and included 31 clinical articles. That review found heterogeneous decolonization results, weak evidence for some bundled preoperative washing contexts, no direct comparative studies of octenidine for pre-incisional skin preparation, and mostly negative evidence for daily octenidine bathing reducing ICU- or catheter-related bloodstream infections.
Two later ICU studies add important context rather than a simple conclusion. A 2023 CLIP-ID post-hoc analysis found no reduction in ICU-attributable CLABSI in the octenidine group, while a 2024 German EFFECT trial reported a reduction in ICU-acquired primary bacteremia with octenidine-impregnated washcloths but no effect on ICU-acquired multidrug-resistant organisms. Those endpoints, study designs, products, and surveillance methods are not interchangeable.
For wound cleansing, the 2023 CADTH review on NCBI Bookshelf summarized wound-cleanser evidence and reported no statistically significant wound-healing difference for octenidine comparisons in the included chronic-wound evidence. It also found no evidence-based guidelines for antimicrobial or antiseptic wound cleansers for wound management in its review question.
Source Scope
Official identity records support identity and synonym statements. The FDA Global Substance Registration System record lists octenidine hydrochloride with synonyms including octenidine dihydrochloride and explicitly notes that a UNII does not imply regulatory review or approval. PubChem and ECHA records are useful identity and substance-context sources, but they do not establish clinical effectiveness, product authorization, body-site suitability, or interchangeability.
Clinical reviews and trials support only the context they studied. Many octenidine sources evaluate finished products, washcloths, gels, decolonization bundles, antiseptic bathing routines, or co-ingredients. Product and formulation context matters; an outcome from one setting is not a general property of octenidine dihydrochloride.
Guidelines and regulator pages are used here as boundary sources. CDC catheter-prevention guidance and the SHEA/IDSA/APIC MRSA practice recommendation are not octenidine endorsement sources. They help show why evidence maps must stay separate from institutional protocols, chlorhexidine-specific recommendations, product labels, and local implementation decisions.
What Every Clinical Claim Must Pin Down
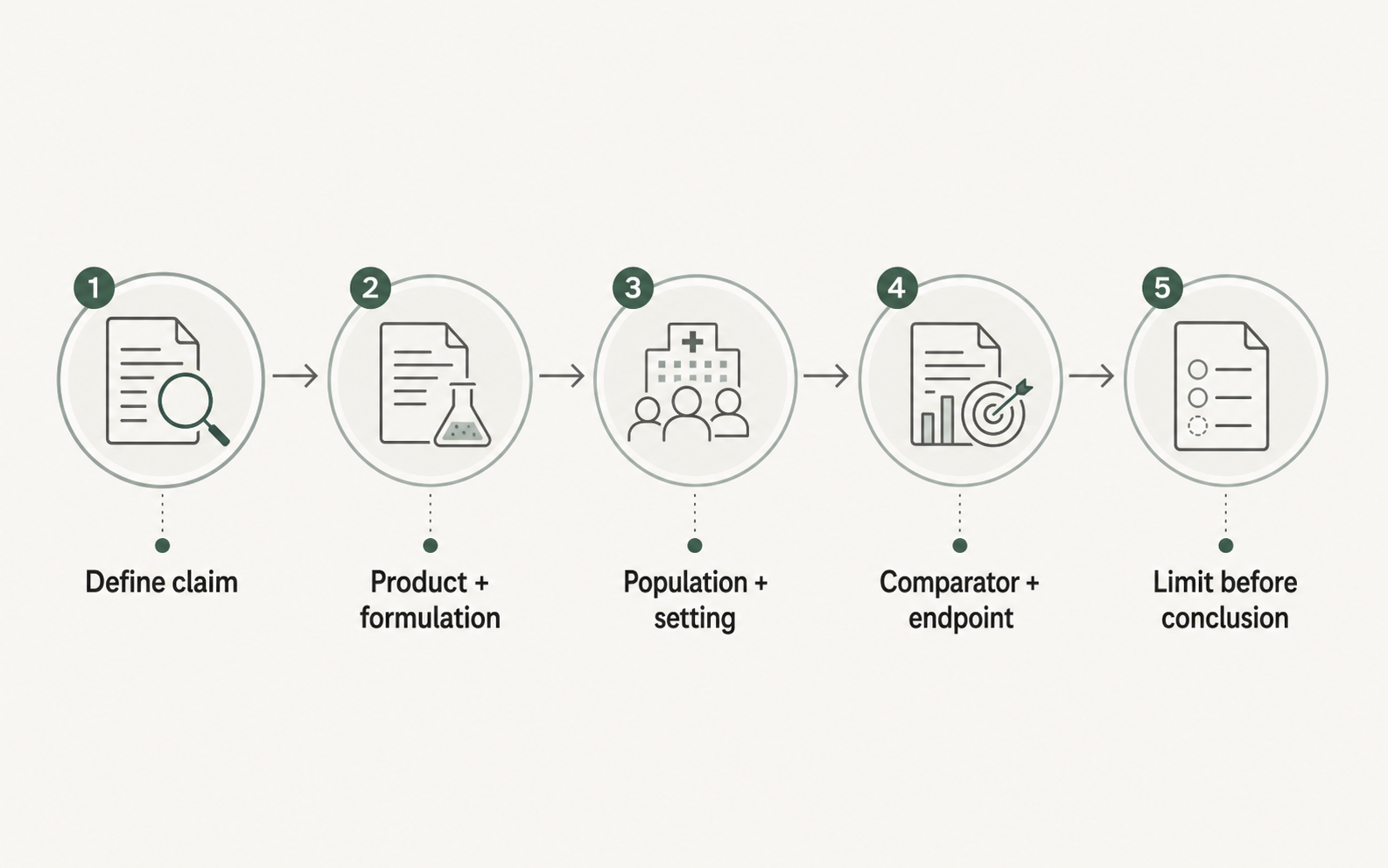
A clinical statement about octenidine dihydrochloride should name the exact claim being made before it names the conclusion.
- Substance or product: octenidine dihydrochloride, octenidine hydrochloride, an octenidine-containing finished product, or a bundle with other measures.
- Formulation and body-site context: skin, nasal, wound, mucosal, catheter-site, whole-body bathing, or another setting.
- Population: adult ICU, surgical cohort, wound type, carrier status, facility type, or other studied group.
- Comparator: saline, Ringer solution, placebo washcloth, water and soap, chlorhexidine, povidone-iodine, bundle care, or no clear comparator.
- Endpoint: colonization, decolonization success, surgical-site infection, CLABSI, ICU-acquired primary bacteremia, wound healing, adverse events, or susceptibility.
- Timing and follow-up: single procedure, short follow-up, 12-month intervention, post-hoc before-after analysis, or systematic review window.
- Jurisdiction and source type: regulator, official substance record, evidence review, guideline, primary trial, or product document.
When one of those fields is missing, the claim is narrower. The missing detail should stay visible rather than be filled by inference.
Evidence Contexts
The safest way to read the literature is by clinical context, not by a single yes-or-no question about octenidine.
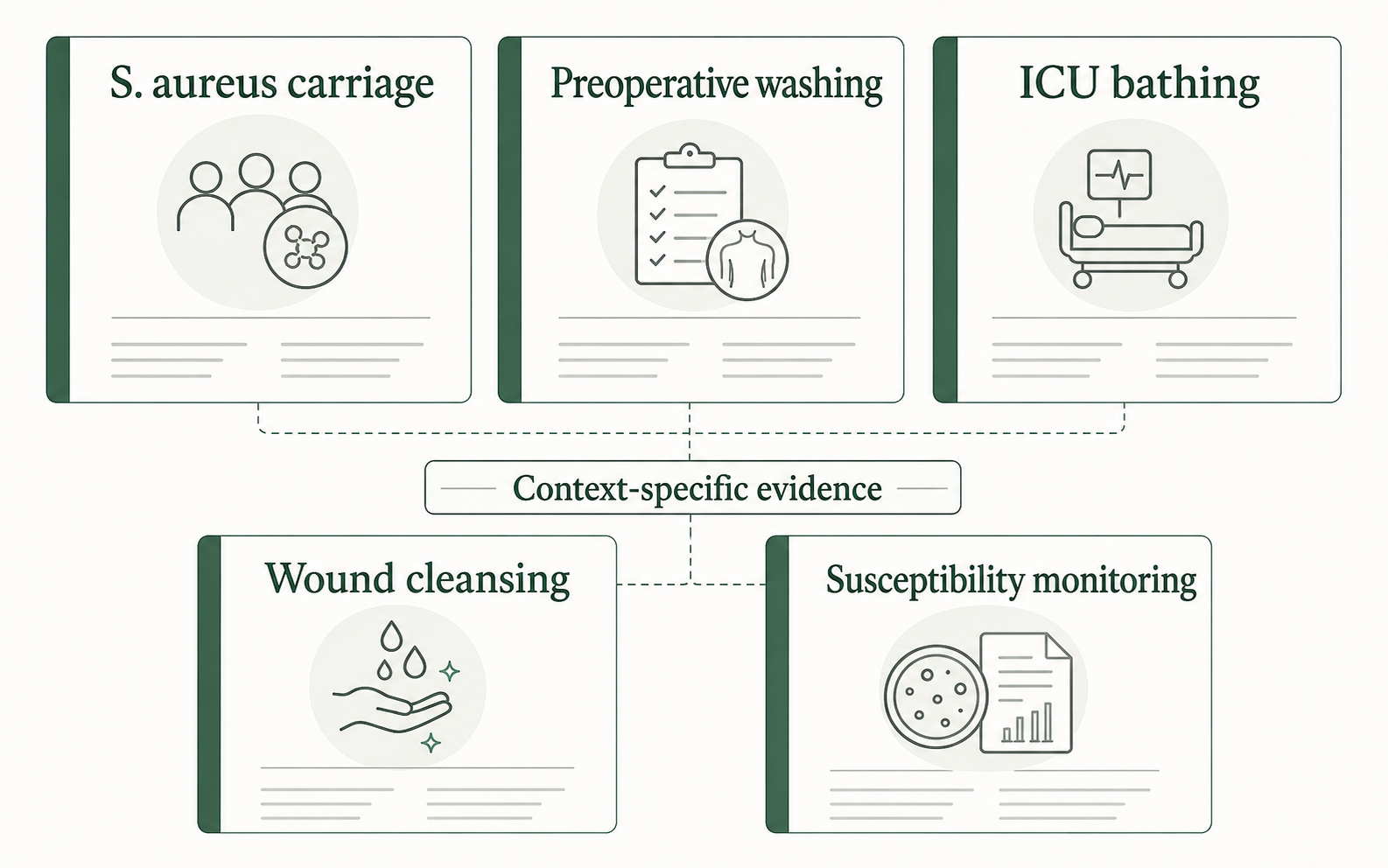
Staphylococcus Aureus Carriage And Decolonization
The 2023 clinical evidence review included studies of octenidine-containing therapies for Staphylococcus aureus carriage or transmission, including MRSA and MSSA contexts. It reported a wide range of decolonization success across studies and noted that single studies showed reductions in S. aureus infection, acquisition, or carriage.
That is not the same as a generalized decolonization recommendation. The review’s findings remain tied to study design, carrier definition, product selection, co-interventions, comparator, site of carriage, and follow-up. The SHEA/IDSA/APIC MRSA practice recommendation is also a useful caution: for that document, MRSA decolonization is framed around intranasal treatment and chlorhexidine skin antisepsis, and the recommendation is not a substitute for individual clinical judgment.
Preoperative Washing And Surgical-Site Infection Outcomes
The 2023 review found weak evidence for octenidine in preoperative washing when combined with other topical measures in orthopedic and cardiac surgery contexts. It also stated that no study compared octenidine for skin preparation before surgical interventions with other antiseptics.
Preoperative washing, pre-incisional skin preparation, and surgical-site infection outcomes should stay separate. A statement about preoperative washing as part of a bundle does not establish that octenidine is preferred for surgical skin preparation, and it does not support substitution for another agent in a local surgical protocol.
ICU Bathing And Bloodstream-Infection Outcomes
The ICU evidence is a good example of why endpoints matter. The 2023 review summarized mostly negative evidence for daily octenidine bathing reducing ICU- or catheter-related bloodstream infections, with one exception in the reviewed literature.
The CLIP-ID post-hoc before-after analysis examined 72 ICUs in Germany and Austria. In the octenidine arm, CLABSI incidence did not decrease when comparing baseline with intervention periods, and the adjusted incidence rate ratio was reported as 1.17 with a 95% confidence interval from 0.79 to 1.72. The same analysis found a reduction in the chlorhexidine group, but that does not create an octenidine substitution statement.
The 2024 EFFECT trial studied 44 ICUs in 23 German hospitals using a cluster-randomized, double-blind, placebo-controlled, cross-over design. It reported a lower hazard of ICU-acquired primary bacteremia with octenidine-impregnated washcloths and no intervention effect for ICU-acquired multidrug-resistant organisms. The article was updated after a 2025 publisher correction to one placebo-event count in Table 2.
Those two ICU sources should be read side by side but not blended. CLABSI, ICU-acquired primary bacteremia, and ICU-acquired MDRO acquisition are different endpoints. A positive signal for one endpoint in one study design does not settle another endpoint, product, population, surveillance method, or implementation question.
Wound Cleansing And Chronic-Wound Evidence
The CADTH wound-cleanser review on NCBI Bookshelf included octenidine among antiseptic wound cleansers in the review scope. For chronic wounds, it summarized included systematic-review evidence in which octenidine comparisons did not show statistically significant differences in complete wound healing, time to complete healing, wound-healing rate, or number of wounds healed, depending on the source comparison.
The same CADTH review did not identify evidence-based guidelines for antimicrobial or antiseptic wound cleansers for wound management, nor studies comparing different antiseptic wound cleansers with one another for that review question. A conservative reading keeps wound evidence tied to wound type, product, comparator, and endpoint rather than treating it as a general instruction to cleanse, irrigate, substitute, or continue a product.
Susceptibility Monitoring And Unintended Consequences
Susceptibility findings should be treated as a separate evidence question from clinical effectiveness. The PLOS ONE analysis from the CLIP-ID trial assessed bacterial isolates from adult ICUs before and after 12 months of routine bathing with chlorhexidine, octenidine, or water and soap. It found no evidence of reduced phenotypic susceptibility to chlorhexidine or octenidine after implementation of the respective antiseptic bathing routines.
The study also cautioned that the 12-month observation period and species-level sample sizes were not enough for final conclusions. Susceptibility data can inform monitoring language, but it should not be used to claim absence of resistance risk, clinical superiority, or long-term ecological safety.
Guideline And Jurisdiction Context
Guideline context matters because octenidine is not the default term in several major U.S.-facing infection-prevention recommendations. CDC catheter guidance names chlorhexidine-containing approaches for several catheter-related prevention practices, including skin preparation and patient cleansing, and includes explicit unresolved or age-specific caution in some pediatric contexts. The SHEA/IDSA/APIC MRSA update similarly frames decolonization around specific agents and implementation decisions, not around a general octenidine class claim.
Octenidine evidence remains useful, but it should not be transformed into U.S. protocol language. A product used in one country, study, or facility should not be treated as authorized or appropriate in another without the relevant product label, regulator source, and local review.
What This Page Does Not Cover
This page does not provide:
- Dosing, application frequency, bathing steps, wound-care steps, catheter-care steps, decolonization regimens, and procedural checklists.
- Claims that octenidine is safer, better, preferred, or interchangeable with chlorhexidine, povidone-iodine, polyhexanide, saline, or any finished product.
- Product-specific directions that lack a current label, jurisdiction, and product-document record.
- Patient-facing advice for wounds, burns, surgical sites, mucosal areas, eyes, ears, infants, pregnancy, breastfeeding, invasive devices, or immunocompromised status.
- Claims that a substance record, supplier page, product availability, or country-specific use establishes clinical approval or medical suitability.
Each conclusion should stay no broader than the source. ICU-acquired primary bacteremia evidence cannot be rewritten as CLABSI prevention. Chronic-wound healing evidence is a different question from surgical-site infection prevention, and a finished-product or bundle outcome cannot be claimed as an isolated active-substance effect.
This page is revisited when major guidelines, labels, systematic reviews, multicenter trials, safety communications, or susceptibility evidence materially change the clinical context.

Sources And Review
This article was editorially reviewed for source traceability and plain-language accuracy on 2026-05-07. Editorial review is not medical advice, regulatory advice, or a clinical recommendation.
Key source categories used:
- Official identity records: FDA GSRS, PubChem, and ECHA, used only for substance identity, synonym, and source-boundary context.
- Evidence reviews: the 2023 clinical review of octenidine in healthcare-associated infection and S. aureus carriage contexts, plus the 2023 CADTH wound-cleanser review on NCBI Bookshelf.
- Primary clinical and surveillance studies: CLIP-ID, EFFECT, and the PLOS ONE susceptibility analysis, used only for their exact populations, products, endpoints, and limitations.
- Guideline context: CDC catheter-prevention recommendations and the SHEA/IDSA/APIC MRSA practice recommendation, used to keep protocol and jurisdiction boundaries visible.
